Your Global Health Resource
Lower Extremity Edema
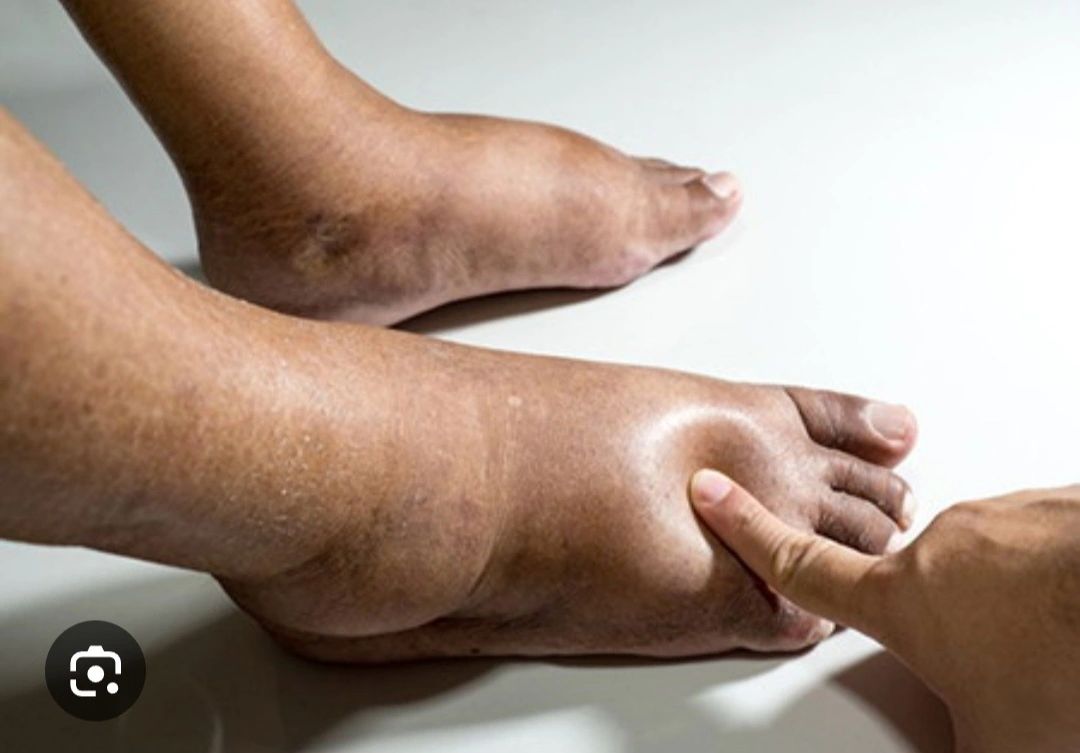
Abstract
Lower extremity edema is a common clinical manifestation with etiologies ranging from benign venous return disorders to potentially life-threatening systemic conditions such as heart failure, thromboembolism, or renal failure. This article reviews the pathophysiology, clinical types of edema, its association with various syndromes, and offers an evidence-based diagnostic and therapeutic approach.
1. Pathophysiology of Edema
Fluid balance between the intravascular, interstitial, and lymphatic compartments is regulated by Starling forces, plasma proteins, capillary integrity, and lymphatic drainage.
Key Mechanisms:
- Increased capillary hydrostatic pressure:
Leads to plasma extravasation into the interstitium.
E.g., venous insufficiency, congestive heart failure (CHF).
- Decreased plasma oncotic pressure:
Reduced fluid reabsorption into the capillaries.
E.g., hypoalbuminemia from nephrosis, liver disease, or malnutrition.
- Increased capillary permeability:
Endothelial injury allows leakage of proteins and fluid.
For example, sepsis, burns, and allergies.
- Lymphatic obstruction (lymphedema):
Impaired drainage of protein-rich interstitial fluid.
- Sodium and water retention:
Related to activation of the renin-angiotensin-aldosterone system or renal dysfunction.
2. Clinical Classification of Edema
By consistency:
- Pitting (soft) edema:
Leaves a depression when pressed.
Common causes: venous insufficiency, hypoalbuminemia, CHF.
- Non-pitting (hard) edema:
Firm consistency, no indentation.
Causes: lymphedema, myxedema.
By distribution:
- Localized:
- Unilateral: DVT, cellulitis, trauma, lymphedema, pelvic aneurysm.
- Bilateral symmetrical: Varicose veins, CHF, pregnancy.
- Unilateral: DVT, cellulitis, trauma, lymphedema, pelvic aneurysm.
- Generalized (anasarca):
Edema involving limbs, face, and serous cavities (ascites, pleural effusion).
Causes: renal failure, cirrhosis, nephrotic syndrome, severe myxedema.
3. Specific Clinical Features and Their Implications
Clinical FeaturePossible EtiologyEdema worsens during the dayChronic venous insufficiencyPersistent morning edemaLymphatic failure, CHFDark or violaceous discolorationChronic venous stasis, dermal hemosiderin depositionTranscutaneous leakage (serous or lymphatic)Advanced edema, lymphedema, cellulitisUnilateral edema + painDVT, cellulitis, compartment syndromeEdema + shortness of breathCHF, PE, nephrotic syndrome with pleural effusionEdema + cognitive declineHepatic encephalopathy, hyponatremia, uremiaEdema + clinical hypothyroidismMyxedema, bradycardia, constipation.
4. Main Clinical Causes of Leg and Foot Edema
- Chronic Venous Insufficiency
Pathophysiology: Venous reflux + venous hypertension
Signs: Varicose veins, ochre pigmentation, malleolar ulcers
- Lymphedema
Primary: Congenital malformations
Secondary: Radiotherapy, lymph node dissection, filariasis
Key sign: Positive Stemmer’s sign
- Congestive Heart Failure (CHF)
Bilateral pitting edema worsens with orthopnea and dyspnea
Reflects elevated venous pressure and neurohormonal activation
- Deep Vein Thrombosis (DVT)
Unilateral edema, pain, warmth, erythema
Risk of pulmonary embolism
- Pulmonary Embolism (PE)
May present with mild edema, sudden dyspnea, pleuritic chest pain
- Nephrotic Syndrome
Generalized edema, periorbital in the morning, severe hypoalbuminemia (<2.5 g/dL), proteinuria >3.5 g/day
- Hepatic Cirrhosis
Portal hypertension + hypoalbuminemia → ascites and leg edema
- Acute or Chronic Renal Failure
Sodium and water retention → anasarca, hypertension, dyspnea
- Myxedema (Severe Hypothyroidism)
Hard, non-pitting edema of the face and limbs
Accompanied by bradycardia, dry skin, macroglossia
- Medications That May Cause Edema:
- Calcium channel blockers (e.g., amlodipine)
- NSAIDs
- Corticosteroids
- Thiazolidinediones (e.g., pioglitazone)
- Tricyclic antidepressants
5. Emergencies and Urgencies Associated with Edema
CauseReason for UrgencyDeep Vein ThrombosisRisk of fatal pulmonary embolismPulmonary EmbolismSudden dyspnea and tachycardiaAcute Heart FailurePulmonary edema, hypoxiaCellulitis on chronic edemaSevere soft tissue infectionCompartment SyndromeAcute tissue ischemiaHepatic encephalopathy/uremiaNeurological compromise
6. Clinical and Paraclinical Diagnosis
Clinical Assessment:
- Detailed history (onset, progression, aggravating factors)
- Focused physical exam: inspection, palpation, pitting, associated signs
Complementary Studies:
TestPurposeVenous Doppler UltrasoundSuspect DVT or venous insufficiencyECG and EchocardiogramAssess ventricular functionRenal function and electrolytesChronic kidney disease, fluid retentionLiver panel and albuminCirrhosis, hypoalbuminemiaTSH and thyroid profileHypothyroidism (myxedema)Urinalysis and 24h proteinuriaNephrotic syndromeBNP or NT-proBNPDecompensated heart failureChest X-rayCardiomegaly, pleural effusionsD-dimerSuggests DVT or PE (guides further testing)
7. Treatment
General Measures:
- Elevate legs above heart level
- Graduated compression stockings (if no DVT)
- Moderate salt restriction
- Weight control and regular physical activity
Pharmacologic Management by Etiology:
CauseTreatmentVenous insufficiencyCompression stockings, leg elevation, phlebotonicsAcute DVTImmediate anticoagulation (heparin or DOAC)CHFLoop diuretics (furosemide), ACE inhibitors, beta-blockers, spironolactoneNephrotic syndromeACE inhibitors/ARBs, immunosuppressants if indicatedCirrhosisSpironolactone ± furosemide, sodium restriction, possible paracentesisHypothyroidismLevothyroxineLymphedemaManual lymphatic drainage, compression therapy, skin care, exercise
8. Prognosis
Prognosis depends on the underlying cause and timeliness of diagnosis:
- Benign: Chronic venous insufficiency, idiopathic edema in young women
- Moderate: Primary or postsurgical lymphedema, hypothyroidism
- Severe to potentially fatal: DVT with PE, decompensated heart, liver, or renal failure
Conclusion
Edema is not a disease but a clinical sign with multiple causes, some of them serious or emergent. Evaluation should be systematic, integrating clinical and laboratory data. Effective treatment depends on early recognition of the underlying etiology and a comprehensive, individualized approach.
RaulAyalaMD
@MyDoctorOnCall.com
